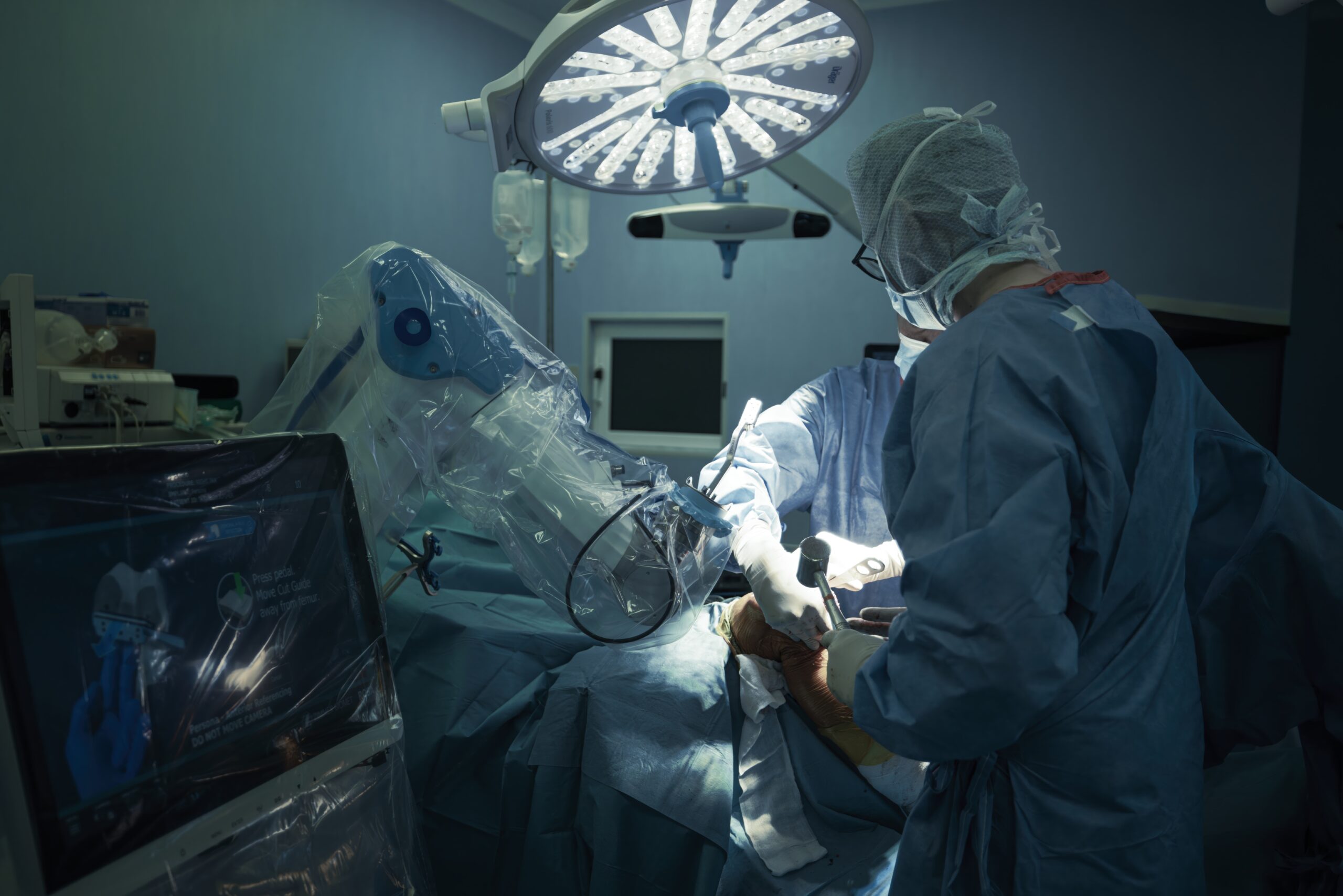
Dr. Omar Marar has witnessed a remarkable transformation in the operating room during his career as a colon and rectal surgeon. From the early expansion of laparoscopic techniques to the refinement of robotic-assisted platforms, surgical practice has shifted toward greater precision, improved visualization, and patient-centered outcomes.
Working at Central Michigan University Health in Saginaw, Michigan, he has observed how technological progress reshapes not only operative technique but also surgical education and patient expectations.
Minimally invasive surgery once represented a dramatic departure from traditional open procedures. Today, robotic innovation is redefining what minimally invasive truly means in colorectal surgery and other complex specialties. The evolution continues, driven by advances in instrumentation, imaging, and surgeon training.
The Transition from Open Surgery to Laparoscopic Precision
The initial movement away from large incisions toward laparoscopic surgery marked a turning point in surgical care. Smaller incisions reduced postoperative pain, shortened hospital stays, and accelerated recovery. For patients undergoing colorectal procedures, these changes were significant.
Complex resections that once required extended hospitalization became more manageable through refined minimally invasive techniques. Laparoscopy introduced surgeons to enhanced camera visualization, though it also presented technical limitations.
Two-dimensional imaging, restricted instrument mobility, and ergonomic strain posed challenges during intricate pelvic dissections. Despite these constraints, laparoscopic surgery laid the foundation for technological integration in the operating room.
The shift demanded adaptation. Surgeons trained in open techniques had to acquire new motor skills and spatial awareness. As fellowship-trained specialists entered practice, minimally invasive approaches gained wider acceptance. Over time, data supporting reduced complications and improved recovery strengthened institutional adoption.
Robotic-Assisted Surgery and the Expansion of Surgical Capability
The arrival of robotic-assisted surgery expanded what minimally invasive techniques could accomplish. Robotic platforms introduced three-dimensional high-definition visualization, tremor filtration, and articulated instruments that mimic the movement of the human wrist. These innovations proved particularly valuable in confined anatomical spaces such as the pelvis.
“Robotic systems allow surgeons to operate with a level of control and visualization that was not previously achievable through standard laparoscopy,” says Dr. Omar Marar. “In colorectal surgery, where precision is critical, that difference matters.”
The ability to perform fine dissection around delicate nerves and vascular structures can influence functional outcomes. In rectal cancer surgery, for example, preservation of autonomic nerves plays an important role in long-term quality of life. Robotic instrumentation offers greater dexterity during these demanding procedures.
Robotic platforms enhance ergonomics for surgeons, so reduced physical strain contributes to consistency across lengthy operations. Fatigue, an often-overlooked variable, can influence performance. Surgical robotics technology addresses that factor by positioning the surgeon at a console with stabilized visualization and intuitive controls.
Impact on Patient Recovery and Clinical Outcomes
Minimally invasive surgery, supported by robotic innovation, has altered the recovery trajectory for many patients. Smaller incisions reduce tissue trauma. Enhanced precision can decrease blood loss. Hospital stays frequently shorten when postoperative pain is controlled and mobilization begins earlier.
“In many cases, patients are surprised at how quickly they are able to resume normal activity after a robotic procedure,” notes Dr. Marar. “The technology supports meticulous technique, and that can translate into smoother postoperative courses.”
Enhanced recovery protocols now complement robotic-assisted colorectal surgery. Coordinated perioperative care, including optimized anesthesia and early nutrition strategies, aligns with minimally invasive approaches. The result is a comprehensive model focused on safety, efficiency, and patient comfort.
Clinical research continues to evaluate long-term oncologic outcomes, complication rates, and cost considerations. While robotic systems require substantial institutional investment, proponents argue that improved visualization and instrument control may reduce conversion to open surgery in complex cases. For patients, the decision often centers on access to experienced surgeons who understand both the technology and its appropriate application.
Training the Next Generation in Robotic Innovation
As an educator and clerkship director, Dr. Omar Marar has observed how surgical training evolves alongside technological progress. Residents and fellows entering the field today encounter robotic platforms as an expected component of operative education. Simulation labs and structured console training have become integral to skill development.
Robotic surgery is not a replacement for sound surgical judgment but a tool that must be integrated into a comprehensive understanding of anatomy, pathology, and patient selection. Training programs increasingly incorporate stepwise credentialing and proctored cases to ensure proficiency.
Mastery requires deliberate practice. Surgeons must learn to troubleshoot equipment, interpret enhanced imaging, and coordinate effectively with operating room teams. Educational institutions face the task of balancing exposure to open, laparoscopic, and robotic techniques.
Each modality retains value. Complex trauma or emergency situations may still require open approaches. Versatility remains essential for surgical competence.
Ethical and Economic Considerations in Surgical Robotics
The expansion of robotic innovation in surgery settings raises questions regarding cost, access, and equitable distribution of care. Robotic systems involve substantial acquisition and maintenance expenses. Hospitals must weigh these investments against measurable clinical benefit.
Discussions include the topic of transparency with patients. Informed consent includes an explanation of available surgical options and the surgeon’s experience with each technique. Clear communication supports shared decision-making.
Technology adoption should align with evidence-based practice. Not every procedure requires robotic assistance. Appropriate case selection preserves resources while maintaining high standards of care. The integration of robotics into colorectal surgery reflects careful evaluation of outcomes over simple enthusiasm for novelty.
“Innovation must be grounded in patient safety and measurable benefit,” explains Dr. Omar Marar. “Technology should enhance surgical capability, not distract from clinical fundamentals.”
The Continuing Evolution of Minimally Invasive Surgery
The trajectory of minimally invasive surgery suggests continued refinement rather than abrupt transformation. Advances in imaging, artificial intelligence integration, and instrument miniaturization are already under development. Future platforms may incorporate augmented reality overlays or improved haptic feedback.
Robotic innovation represents a milestone in that progression. It builds upon decades of surgical advancement, specifically in colorectal care, while introducing capabilities that expand technical precision. As research accumulates, clinical guidelines will adapt to incorporate validated benefits.
The operating room today differs markedly from that of a generation ago. Surgeons collaborate with engineers, data scientists, and device manufacturers to refine systems that improve accuracy and workflow. For specialists in colon and rectal surgery, these developments influence cancer care, inflammatory bowel disease management, and complex reconstructive procedures.
The evolution of minimally invasive surgery through robotic innovation reflects a broader pattern in medicine. Progress occurs through incremental improvement, disciplined evaluation, and sustained commitment to patient welfare. Surgical robotics technology continues to shape that path, offering tools that enhance precision while preserving the foundational principles of operative care.
As minimally invasive techniques advance, the emphasis stays focused on thoughtful application, rigorous training, and measurable outcomes. The future of robotic-assisted surgery will depend on hardware sophistication but, more importantly, on the expertise of surgeons who integrate innovation with clinical judgment.