Over two decades of research, from cross-sectional studies to large randomized trials, keeps pointing to the same thing: the health of your gums and the health of your heart are far more connected than most people know.
Nearly 42% of American adults over 30 have some form of periodontal disease. Many of them have no idea. They do not feel serious pain. They may notice a little blood when they brush. They move on. But inside their bodies, a slow fire of inflammation is burning, and that fire may be feeding one of the most dangerous diseases in the country.
Cardiovascular disease kills more Americans each year than cancer and chronic lung disease combined. In 2020 alone, nearly 929,000 deaths in the United States were linked to atherosclerotic cardiovascular disease. The economic cost reached $407 billion between 2018 and 2019.
Doctors and researchers are now taking a hard look at gum disease as one of the contributing factors. Here is what the science says, what it means for you, and what you can do right now.
What Periodontal Disease Actually Is
Periodontal disease is not just bad breath or sensitive gums. It is a chronic inflammatory infection. It starts when bacteria in your mouth form a film on your teeth called plaque. If that plaque is not removed, it hardens into tartar, and bacteria go deeper.
In the early stage, called gingivitis, gums become red and swollen. They may bleed when you brush. At this point, the damage is reversible with good care.
If ignored, gingivitis becomes periodontitis. The infection spreads below the gum line. It starts destroying the tissue and bone that hold your teeth in place. Pockets form around the teeth. Bacteria settle in those pockets. Teeth can become loose. They can fall out.
Periodontitis is ranked the sixth most common disease in humans worldwide. It affects an estimated 740 million people globally. In the United States, 7.8% of adults have the severe form.
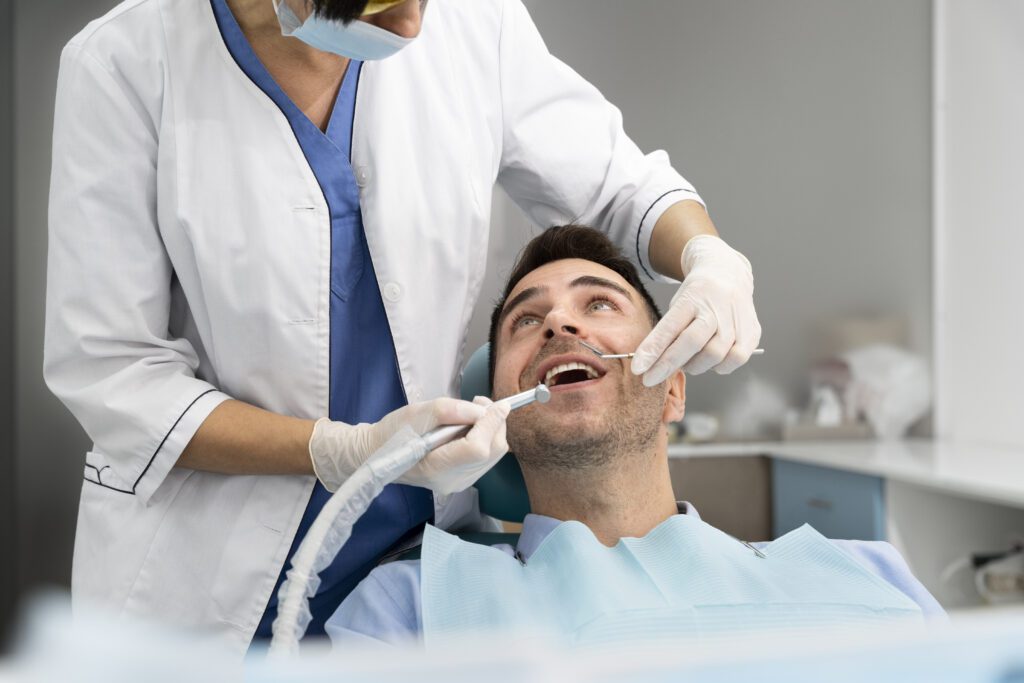
The team at Dental Faith in Nashville offers periodontal therapy as part of their preventive care. Catching and treating gum disease early is one of the most important steps you can take, not just for your mouth, but for your whole body.
The Heart Disease Problem
Atherosclerotic cardiovascular disease, or ASCVD, is an umbrella term. It includes coronary artery disease, heart attack, stroke, and peripheral artery disease. All of these involve plaque building up inside blood vessels over time.
That plaque is not the same as dental plaque. Arterial plaque is made of fat, cholesterol, calcium, and other materials. As it builds up, arteries narrow. Blood flow slows. The heart works harder. Eventually, a clot can form. A heart attack or stroke follows.
About 605,000 new heart attacks happen every year in the United States. Another 200,000 are recurrent attacks in people who already had one. Strokes account for roughly 1 in every 21 deaths.
Doctors have long focused on the known risk factors: smoking, high blood pressure, high cholesterol, diabetes, obesity, and physical inactivity. These are all real. But a growing body of evidence says chronic infections and inflammation, including the kind that comes from gum disease, may be part of the equation too.
What the Research Shows
The American Heart Association published a major scientific statement on this topic. The conclusion was clear: there is consistent evidence of an association between periodontal disease and cardiovascular disease. That statement has been updated as new research has come in, and the evidence has only grown stronger.
Multiple meta-analyses and systematic reviews have found that people with periodontal disease are at higher risk for heart events. One meta-analysis found that chronic periodontitis patients had a 19% higher risk of developing cardiovascular events. People under 65 were at even higher risk, nearly 44% above average.
Another large analysis combining seven cohort studies found that individuals with periodontitis had about a 34% higher chance of developing cardiovascular disease compared to those without gum disease.
A 13-year follow-up study published in recent years found that severe periodontitis was independently linked to a higher rate of coronary heart disease, even after accounting for existing cardiovascular risk factors.
Studies on stroke tell a similar story. Several meta-analyses confirm that periodontal disease significantly raises the risk for stroke. For people who have already had a stroke, having gum disease also increases the risk of having another one.
Beyond stroke and heart attack, gum disease has also been linked to atrial fibrillation, heart failure, peripheral artery disease, and hypertension. It has also been associated with type 2 diabetes, obesity, and chronic kidney disease.
This does not mean gum disease causes all of these. Researchers are still working to establish causation. But the associations are consistent, and they have been replicated across dozens of countries and study designs.
How Gum Disease Affects the Heart: Two Main Pathways
Researchers have proposed two main ways that periodontal disease may influence cardiovascular health.
The Direct Path: Bacteria in the Blood
Every time you chew, brush, or have a dental procedure, bacteria from infected gum pockets can enter your bloodstream. This is called bacteremia. In healthy people with healthy gums, this is brief and harmless. But in someone with severe periodontal disease, it happens repeatedly, and the bacteria are more dangerous.
Specific periodontal bacteria, particularly Porphyromonas gingivalis, have been found inside arterial plaque in heart patients. These organisms can invade the cells that line blood vessels, causing local inflammation and contributing to the buildup of plaque inside arteries.
Studies have isolated live periodontal pathogens from atherosclerotic tissue samples. In animal models, oral infection with these same bacteria has been shown to promote atherosclerosis. The evidence across multiple species, including rodents, rabbits, and pigs, is substantial.
The Indirect Path: Chronic Systemic Inflammation
The second pathway is inflammation. Periodontal disease creates a constant low-grade inflammatory state in the body. It raises circulating levels of CRP, also called C-reactive protein, which is one of the most widely used markers of cardiovascular risk.
It also elevates interleukin-1, interleukin-6, interleukin-8, and tumor necrosis factor. All of these inflammatory proteins are known to be associated with coronary heart disease. They accelerate the process of atherosclerosis by acting on blood vessel walls, increasing oxidative stress, and disrupting normal lipid metabolism.
Patients with periodontal disease also show elevated platelet activation. Platelets play a central role in clot formation. Overactive platelets raise the risk of the kind of clot that causes a heart attack or stroke.
Additionally, there is evidence of a shared genetic link. A genetic region on chromosome 9p21.3, known to be one of the strongest cardiovascular risk loci, has also been associated with periodontal disease. This suggests that some people may carry a biological predisposition to both conditions.
What Happens Under the Surface: Subclinical Signs
Before a heart attack or stroke, damage is already happening at a level you cannot feel. Researchers have found that gum disease is linked to several early warning signs of vascular disease.
Carotid intima-media thickness, or CIMT, is a measure of how thick the walls of the carotid arteries are. Thicker walls are an early sign of atherosclerosis. Studies show that people with periodontal disease have significantly higher CIMT. Severe gum disease increases the odds of thickened CIMT by 70% compared to people without gum disease.
Endothelial function is another early marker. The endothelium is the inner lining of blood vessels. When it works well, blood flows freely. When it does not, clots and blockages form more easily. A meta-analysis found significantly reduced endothelial function in people with periodontal disease.
Arterial stiffness is also higher in people with severe gum disease. Stiff arteries force the heart to work harder and are associated with organ damage over time, including damage to the kidneys and brain.
Can Treating Gum Disease Help the Heart?
This is where science is still developing. Proving that treating gum disease actually prevents heart attacks requires large, long-term randomized trials. Those take years and cost a great deal. The studies that exist so far are promising but not yet definitive.
Preventive care models, such as the BaleDoneen Method, take a broader view by assessing both arterial health and inflammatory factors, including oral health. In this approach, gum disease is considered one of several possible contributors to artery inflammation that may influence heart attack risk, though ongoing research continues to clarify the strength of this link.
What is clear is that treating periodontal disease improves the intermediate markers that raise cardiovascular risk. Several randomized controlled trials have shown that scaling and root planing, the main non-surgical treatment for gum disease, significantly reduces CRP levels in the blood.
One trial of patients with confirmed coronary heart disease found that periodontal treatment significantly lowered CRP, fibrinogen, and white blood cell counts. These are all markers of systemic inflammation that contribute to heart disease progression.
A large analysis found that periodontal treatment improved total cholesterol, triglyceride levels, and HDL cholesterol. Studies have also found improvements in blood pressure, particularly in patients who already had hypertension. Endothelial function improved in patients with cardiovascular disease or diabetes after periodontal treatment.
One study tracking 13,761 adults found that the estimated 10-year cardiovascular risk dropped significantly with increased frequency of tooth brushing. Brushing three or more times per day was associated with nearly half the estimated risk compared to brushing once a day or less.
The broader picture is this: treating gum disease will not replace heart medication or reverse existing artery damage. But it reduces the inflammatory burden that feeds cardiovascular disease. That matters.
Who Is at the Highest Risk?
Some people face a higher combined risk from both conditions. Research shows that males and people with severe periodontal disease are at the highest cardiovascular risk from this association.
You may also be at elevated risk if you are over 65, have diabetes, smoke, have high blood pressure, or have a lower income. Poverty is strongly tied to both gum disease and heart disease. The prevalence of severe periodontitis reaches 60% in people earning below the federal poverty level.
People who have already had a heart attack or stroke need to be especially aware. Periodontal disease raises the risk of a second cardiovascular event. It is not enough to manage cholesterol and blood pressure. Oral health needs to be part of the picture.
Interestingly, children are not off the hook. Studies from the Cardiovascular Risk in Young Finns Study found that oral infections in childhood predicted subclinical atherosclerosis in adulthood. Adolescents with gum disease show higher inflammatory markers and elevated diastolic blood pressure. Early dental care matters for long-term heart health.
What You Should Do About This
Get a full periodontal exam
Ask your dentist to check the depth of the pockets around your teeth. Healthy pockets measure 1 to 3 mm. Anything deeper signals disease. If you have not had this exam recently, ask for it by name.
Do not skip professional cleanings
Brushing and flossing at home do not remove hardened tartar below the gum line. Professional cleanings do. People with active gum disease usually need cleanings every three to four months, not just twice a year.
Brush more, and brush better
Research links brushing frequency directly to lower cardiovascular risk markers. Brushing twice a day at minimum, preferably three times, with a soft brush and proper technique, makes a measurable difference.
Floss every single day
Most people skip flossing. Flossing removes bacteria from between teeth that a brush cannot reach. It is one of the most underrated health habits you have.
Tell your dentist about your heart history
If you take blood thinners, have had a heart procedure, have a pacemaker, or have any heart condition, your dentist needs to know. It changes how they approach treatment and anesthesia.
Tell your cardiologist about your gums
Most cardiologists do not routinely ask about oral health. Bring it up. If you are working with a specialist in cardiovascular prevention and risk reduction, your gum health is part of your inflammation profile. Comprehensive prevention programs are increasingly looking at oral health as a measurable risk factor, not a side note.
Manage your shared risk factors
Smoking damages both your gums and your arteries. Quitting is the single most effective thing a smoker can do for both. Controlling blood sugar if you have diabetes, keeping blood pressure in a healthy range, and eating a diet low in processed foods all reduce risk on both fronts.
What the Research Still Needs to Prove
The association between periodontal disease and cardiovascular disease is well established. Causation is not. Most major health organizations, including the American Heart Association, acknowledge that current evidence does not definitively prove gum disease causes heart disease.
What it does show is that the two conditions share biological pathways, common risk factors, and a consistent pattern of co-occurrence that cannot be explained away by chance or lifestyle factors alone.
Ongoing research using Mendelian randomization, which uses genetic data to test causal relationships, has found some links between genetic markers of periodontal disease and cardiovascular outcomes. But results are mixed, and more work is needed.
Larger, better-funded clinical trials are now underway to test whether treating gum disease directly reduces cardiovascular events. The early data is encouraging. The complete picture will take years to fully confirm.
The Bottom Line
Heart disease is the leading cause of death in the United States. It is responsible for more deaths than the next two causes combined. Gum disease affects nearly half of all American adults. These are not isolated problems.
The science makes a clear case: your mouth is not separate from your cardiovascular system. The bacteria in your gum pockets, the inflammation they generate, and the signals they send through your bloodstream all affect what happens in your heart and arteries.
You do not need to wait for the final word from researchers to act. The steps that protect your gums also reduce your cardiovascular risk. See your dentist. Treat active gum disease. Brush and floss. And make sure the people managing your heart health know about the state of your mouth.
Prevention is always more effective than treatment. The mouth is a good place to start.